How long it takes for TMS to work often comes down to how a patient’s brain responds to steady, targeted stimulation, and most people begin noticing changes somewhere between the fourth and sixth week of treatment.
TMS uses magnetic pulses to reach mood‑related regions about a few centimeters beneath the scalp, and sessions run around 20 minutes, five days a week, which creates a steady rhythm the brain can adapt to.
Some patients sense small shifts by week two, though the fuller response usually settles in later as the circuit pathways adjust. If you’re weighing this therapy, keep reading to see how the process unfolds.
Key Takeaway
- Standard TMS courses usually span 30–36 sessions over about 4–6 weeks.
- Some patients may notice early symptom easing after roughly 2 weeks, though fuller effects tend to appear once the series is completed.
- Periodic maintenance sessions can help stabilize gains and support longer term symptom control.
Typical TMS Treatment Timeline
The first phase at TMS Tennessee usually runs on a steady rhythm, daily visits, five days a week, carried out over 4–6 weeks depending on how the plan is shaped for each person. The structure stays consistent, mostly because the brain responds best to repeated stimulation at regular intervals.
Patients can expect:
- Sessions lasting about 20 minutes
- A total of 30–36 sessions, spaced across the initial weeks
- In‑office treatment only, without sedation or anesthesia
Some people mention small shifts in mood or less tension after the second week, although the broader change tends to build slowly and doesn’t usually settle in until the full course is finished.
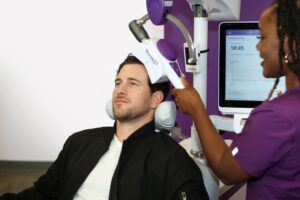
What Happens During Each Session?
The NeuroStar system sends controlled magnetic pulses toward areas of the brain tied to mood regulation. It’s a non‑invasive process, and while the pulses might cause brief discomfort on the scalp, most patients ease into the pattern after the first few sessions.
A typical visit includes:
- A personalized setup guided by brain‑mapping measurements
- Staying awake and alert the whole time
- No recovery period, so you can return to regular activities right away
These appointments depend a lot on consistency, and missing too many can slow the overall response, which is why we encourage keeping the schedule as steady as possible.
Factors Influencing the Timeline for TMS Effectiveness

Individual Patient Conditions
When a person walks in with heavier symptom loads, especially major depressive episodes or long running anxiety the brain often needs more repetition before it responds. Patients dealing with treatment‑resistant depression might end up moving through the full 6‑week plan, sometimes even a bit longer, before they notice clearer relief. You can see how the brain, being cautious, takes its time.
Specific Treatment Protocols
NeuroStar systems allow clinicians to choose from several stimulation patterns. Some clinicians use standard repetitive TMS (TMS), which relies on steady pulses over about 18–20 minutes.
Others might use theta burst (a faster pattern delivered in tight clusters at higher frequency, lasting only a few minutes). That choice can shift the pace of symptom change; shorter sessions with denser pulses might lead to earlier improvements, though not everyone responds the same, and we all weigh those options case by case.
Treatment Consistency
TMS works through gradual neural training, so the weekly rhythm, usually 5 sessions every week for several weeks really matters. Missing sessions breaks that rhythm, which might stretch the timeline or dull the overall response, and most clinicians try to keep the schedule steady so the brain doesn’t lose momentum between sessions.
Summary of Influencing Factors:
- Symptom severity and diagnosis
- TMS protocol specifics
- Session attendance and patient compliance
Keeping a steady schedule tends to give patients the best chance for earlier, more noticeable improvement.
The Tapering Phase and Extended Treatment
We keep noticing how tapering works a bit like easing off a tight brace, giving the brain room to settle without losing ground.
- Some patients move into a tapering phase after the first intensive stretch, a pattern that mirrors what’s outlined in this treatment progression guide, and it usually means fewer sessions spread out in a steady, predictable way.
- This tapering period can stretch the full treatment to about 9 weeks, which might sound long, though it often helps the brain keep the gains it’s made.
- The goal is to hold those improvements in place while lowering the chance the symptoms slip back.
- Not every patient needs tapering, and the choice is made case by case, often after we look at how stable the response has been.
- Tapering works as a bridge rather than a stop, letting patients shift toward long‑term maintenance without feeling abruptly cut off.
Duration of TMS Effects and Maintenance Sessions

We’ve seen how the first stretch of TMS can steady a person in ways that feel almost quiet at first, then clearer as weeks pass.
Many patients keep those gains for several months, and studies show that around 50–60 percent hold onto noticeable relief for close to a year, sometimes longer, a pattern echoed in this long-term outcomes summary, though it varies from one person to the next.
Why Maintenance Sessions Matter
Some people return for booster sessions because symptoms can drift back, even slowly. These visits might be set monthly, or every few months, depending on how someone responds and how steady their mood stays between sessions. [1]
At TMS of Tennessee, we check in often, adjusting plans when the pattern of symptoms shifts, since a small change in timing can help keep the treatment’s effect stable.
Long Term Outlook
The long term course of TMS [2] usually depends on a few pieces working together, such as:
- A person’s medical and psychiatric history
- Daily pressures, sleep routines, and stress
- Ongoing care with a therapist or psychiatrist
When someone pairs TMS with steadier habits and regular counseling, the relief tends to last longer, and the symptoms don’t swing as sharply. It’s not a fixed rule, but the pattern shows up often enough that we pay attention to it.
Maximizing the Benefits of TMS Therapy
- Optimal outcomes usually come when the care plan extends beyond the magnetic stimulation itself.
- Follow‑up visits with a mental health clinician help patients sort through changes in mood and offer steady support.
- Healthy routines, regular exercise, a balanced diet, and consistent sleep tend to work alongside TMS and strengthen its effect.
- When appropriate, TMS can be paired with psychotherapy or medication, and this combination might guide some patients toward steadier symptom relief.
TMS of Tennessee develops individualized treatment plans and monitors patients closely so the therapy can be adjusted to match each person’s clinical needs.
Summarizing the TMS Treatment Timeline and Outcomes
- Most treatment plans run about 4 to 6 weeks, adding up to 30 to 36 sessions, and the steady pace often helps the brain settle into the work.
- Each visit lasts around 20 minutes, usually five days a week, which can feel routine after the first few sessions.
- Some people notice small shifts after 2 weeks, though the full effect usually appears once the main course is done, and it’s normal for progress to rise in steps rather than a straight line.
- A taper phase, which might stretch the plan to 9 weeks, gives the brain a slower landing and can be useful for patients who respond more gradually.
- Maintenance sessions, spaced farther apart, often help keep symptoms controlled for months or even years, depending on how each person responds.
- Sticking to the schedule, along with steady sleep, movement, and support at home, probably strengthens the treatment’s overall impact, even if the changes feel subtle at first.
FAQ
How long does TMS therapy take to show results, and what affects the TMS treatment duration or TMS treatment timeline?
People often ask how long does TMS take to work because the first changes can feel slow. Most folks see TMS symptom improvement after a few weeks, but the TMS patient response varies. The TMS session length, TMS sessions per week, and your TMS protocol weeks all shape how fast things shift.
Some notice rapid TMS effects, while others see gradual improvement. Your care team may adjust TMS treatment frequency or TMS coil placement to guide better TMS outcomes.
What should I expect from TMS depression treatment in terms of TMS effectiveness, TMS symptom relief, and TMS depression remission?
With TMS depression treatment, many people feel steady TMS mood improvement as TMS brain stimulation supports healthy TMS neuroplasticity. The pace of TMS symptom relief depends on factors like TMS repetitive sessions, TMS brain regions, and the chosen TMS protocol or theta burst stimulation.
Research shows solid TMS remission rates, but TMS outcomes variability is normal. Some may need a TMS tapering phase or later TMS maintenance sessions to keep gains.
How safe is Transcranial Magnetic Stimulation, and what should I know about TMS side effects or TMS treatment risks?
Most people tolerate Transcranial Magnetic Stimulation well, and TMS treatment safety is backed by TMS FDA approval and many TMS research studies. Common TMS therapy side effects are mild and short term. Providers track TMS patient care and may adjust TMS magnetic coil settings to ease issues.
Serious TMS treatment risks are rare. There’s usually little TMS recovery time, and the TMS session experience is simple: brief TMS magnetic pulses to targeted areas using careful TMS brain targeting.
How do different TMS treatment plans affect long term progress, including TMS long term effects or duration of TMS effect?
Your TMS treatment plans guide both short term change and TMS long term effects. Some people benefit from accelerated TMS, an accelerated TMS protocol, or personalized TMS targeting when symptoms run deep, such as in TMS for treatment resistant depression, TMS for anxiety, or TMS for OCD.
Over time, TMS brain plasticity can support lasting gains. Many rely on a TMS treatment booster later on. Care teams use TMS outcome tracking, TMS symptom monitoring, and TMS clinical effectiveness data to shape your path.
Conclusion
We keep thinking about how the room gets quiet when someone finally feels a bit lighter, and it reminds us why TMS might matter to you, or anyone who’s been stuck in the dark too long.
The NeuroStar sessions in Franklin work with steady magnetic pulses, about 19 minutes at a time, nudging those quieter brain pathways awake, and the pace of change can feel steady but real. If you’re considering a non‑drug path that fits into regular routines, this might be the step that helps.
Schedule your consultation at TMS of Tennessee and see if this approach fits your next move.