Is TMS therapy safe? The short answer is yes. When someone’s dealing with depression that just won’t budge, TMS stands out as one of the safer options available in mental health treatment.
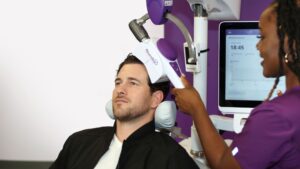
Picture this: magnetic pulses, similar to what’s used in MRI machines (but more targeted), stimulating specific parts of the brain. No surgery, no anesthesia, patients walk in and out of their doctor’s office in about 40 minutes. While it might sound a bit sci-fi, medical professionals have been using TMS since the 1980s, and thousands of patients have found relief without major complications. But like any medical procedure, there’s more to the story.
Let’s look at what makes TMS tick and what patients should keep in mind.
Key Takeaways
- TMS therapy stands out as a non-invasive option that’s gotten the FDA-cleared with years of safety data behind it
- Some people may deal with minor stuff like scalp tenderness or headaches that go away pretty quick
- Individuals with certain metal implants or a history of seizures require careful evaluation before TMS, and treatment may be contraindicated depending on the device type or seizure control status.
What’s TMS All About?
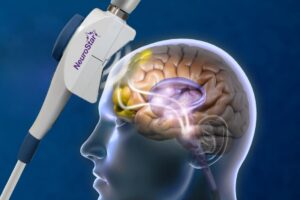
The brain’s a complex piece of machinery, and TMS (that’s Transcranial Magnetic Stimulation) works by sending magnetic pulses right through the skull to wake up specific parts of the brain. It’s primarily used when depression hits hard, though doctors have found it may help with other mental health challenges too.
Think of it like a highly targeted reset button, the magnetic coil sits on your head and delivers these pulses to the prefrontal cortex, where a lot of our mood regulation happens, especially when administered with NeuroStar Advanced TMS Therapy.
When the usual suspects, antidepressants and therapy sessions, aren’t cutting it anymore, that’s when TMS typically enters the picture. The whole thing takes maybe 20-40 minutes, tops, and you can walk right out of the clinic afterward. No overnight stays, no fuss.
- The treatment zeros in on this spot called the dorsolateral prefrontal cortex (doesn’t exactly roll off the tongue, does it?), where it gets those nerve cells firing
- It’s kind of like ECT’s younger, gentler cousin, no need for anesthesia, and you won’t have any seizures
- You’ll need to stick with it, though, we’re talking multiple sessions over several weeks to get the best shot at improvement

The Short Answer: Safe Overall
When patients hear about magnetic pulses going into their brain, they get nervous, and that’s normal. But here’s the reality: TMS doesn’t need cutting, doesn’t knock you out, and doesn’t require any recovery time. You’ll walk in, sit through the session, and drive yourself home. For folks who’ve tried antidepressants without success, it’s proven particularly valuable.
The FDA-cleared TMS devices after extensive clinical trials demonstrating safety and efficacy for treatment-resistant depression. Most patients just feel a light tapping sensation, maybe some tingling where the coil touches their scalp. Nothing major, and it fades fast.
Breaking Down the Safety Factors
No Cutting Required
The whole thing’s external, we’re talking about a magnetic coil that sits right on your head. Those magnetic pulses pass through the skull without causing pain. Since you’re awake the entire time:
- No worrying about anesthesia complications
- No hospital stays
- No recovery period
- No full-body medication side effects
FDA-Cleared
The FDA didn’t just rubber-stamp these devices. They put them through extensive clinical trials for depression treatment, running the numbers on thousands of patients before saying “cleared.”
Targeted Treatment
Unlike pills that flood your whole system, TMS zeros in on specific brain regions. That means you’re not dealing with the usual medication headaches, no weight changes, no nausea, no sexual side effects.
Long-Term Data Looks Good
We’ve tracked patients for years now, and the data’s encouraging. Long-term studies have found no evidence of brain damage or cognitive decline with repeated TMS treatments, though ongoing monitoring and research continue to ensure safety. Some patients come back for touch-up sessions when needed, and we’re not seeing any increased risks.
A 2023 meta-analysis involving over 3,000 subjects reported that most adverse events were mild and transient, with a low risk of serious adverse events including seizures and mood switches. [2]
Potential Risks and Side Effects
The Usual Suspects (Mild and Short-Lived)
Most patients walk away with minimal issues:
- Patients often feel light tapping on the scalp and may experience headaches, which are usually mild and resolve quickly after treatment.
- Face muscles might twitch a bit, totally normal when those magnetic pulses hit the nerve endings
- A few patients may experience mild dizziness during or shortly after treatment, which typically resolves on its own.
- A couple Tylenol usually takes care of any discomfort, and these issues tend to fade after the first few visits
The Serious Stuff (Rare but Worth Knowing)
Let’s be straight about the heavy hitters:
- Seizures are the big one, we’re talking less than 1 in 1000 patients, and usually only in folks who already have epilepsy or past brain injuries.
- Patients with bipolar disorder may be at risk of a manic episode, so TMS should only be administered under careful psychiatric supervision.
Putting Risk in Perspective
These major complications? Pretty rare, and they typically show up in patients who’ve got other health issues going on. The minor stuff usually clears up on its own.
Who Needs to Skip TMS? (Deal-Breakers)
- Individuals with metal implants in the head (excluding most dental work) should not undergo TMS due to potential interference with the magnetic field.
- Pacemakers or cochlear implants? Sorry, can’t risk those devices going haywire
- History of seizures or certain brain conditions? We’ll need to take a really close look before giving the green light
- Brain tumors, stroke history, or previous head injuries? Your doctor’s going to need to do some serious homework before considering this treatment
Why You Need the Professionals for TMS Treatment
Let’s be clear, TMS isn’t something you can DIY in your garage. It takes skilled medical staff who know exactly what they’re doing. Before anyone gets near that magnetic coil, they’ll run through a detailed screening process at specialized Psychiatric Services clinics. They’ll figure out your motor threshold, basically, the sweet spot for magnetic strength that works best for your brain.
These doctors keep a close eye on everything during treatment. If something’s not quite right, they’ll adjust the settings or change up the schedule. That’s exactly why TMS has such solid safety numbers, there’s always a professional watching your back.

Getting Real About Your Options
Listen, if TMS is on your radar, you need to sit down with a qualified doctor. Places like TMS of Tennessee employ specialists who’ve seen hundreds of cases. Come prepared to lay it all out, your mental health background, any metal bits in your body, nerve issues, what treatments worked (or didn’t) before.
Your doctor will walk you through everything, good and bad, so you can make the call that’s right for you. No pressure, just straight talk about whether TMS for Depression or other targeted therapies make sense for your situation.
Remember, it’s your brain we’re talking about here. Take the time to get answers to every single question you’ve got. A good doctor expects that and won’t rush you through the decision.
FAQ
Can repetitive transcranial magnetic stimulation cause cognitive side effects or interfere with brain imaging scans in patients with a history of head trauma or cerebrovascular disease?
Patients with past head trauma or cerebrovascular disease often worry whether repetitive TMS or Deep TMS™ could affect brain function or interfere with brain imaging scans. While most studies show a favorable safety profile, scalp discomfort, site pain, or minor jaw pain may occur.
Staff training and careful dosage selection are essential to minimize risks, especially for those undergoing neuropsychological tasks or fMRI-guided theta burst stimulation in a clinical setting.
How does the presence of metal plates, magnetic implants, or implantable devices like cardioverter defibrillators influence the safety of TMS therapy?
Magnetic implants, metal plates, or implantable devices may interact with the electromagnetic coil during repetitive transcranial magnetic stimulation. Deep brain stimulators and implantable devices require careful evaluation before treatment sessions.
Safety protocols include brain imaging scans, motor threshold determination, and staff training to prevent adverse events such as localized heating or interference with device function. A thorough mental health evaluation and medical information review are required in the United States clinical setting.
Is repetitive TMS safe for patients with seizure disorder, bipolar depression, or post-stroke depression undergoing Theta Burst Stimulation or the SAINT™ protocol?
Individuals with seizure disorder, bipolar depression, or post-stroke depression may have heightened concerns about generalized tonic-clonic seizure risks during intermittent theta-burst stimulation or SAINT™ protocol sessions.
Evidence indicates repetitive TMS and Theta Burst Stimulation have a strong safety profile when administered in a clinical setting. Staff monitor response rates, motor hotspots, and motor threshold determination to reduce seizure risk, with treatment sessions adapted to individual brain stimulation needs, including Accelerated TMS protocols designed for intensive, short-duration treatment plans.
What precautions are needed for patients with major depressive disorder, obsessive-compulsive disorder, or post-traumatic stress disorder using figure-eight coils or deep TMS™ in outpatient procedures?
Patients with major depressive disorder, obsessive-compulsive disorder, or post-traumatic stress disorder often undergo repetitive TMS in an outpatient procedure. Using figure-eight coils or Deep TMS™, practitioners monitor scalp discomfort, site pain, and auditory canal effects.
Safety measures include neuropsychological tasks, serum drug testing, and urine drug testing, while combining with cognitive behavioral therapy may improve outcomes. Proper staff training ensures minimal cognitive side effects and optimal brain stimulation targeting the left frontal cortex.
Can repetitive transcranial magnetic stimulation safely coexist with other treatments like electroconvulsive therapy, vagus nerve stimulation, or medications in patients with Parkinson’s disease, multiple sclerosis, or cerebrovascular disease?
Patients with Parkinson’s disease, multiple sclerosis, or cerebrovascular disease may already use electroconvulsive therapy, vagus nerve stimulation, or medications that affect brain function. Repetitive TMS therapy sessions require careful evaluation of magnetic energy exposure, implantable devices, and potential interaction with other interventions.
Clinical guidelines by the Clinical TMS Society, International Federation of Clinical Neurophysiology, and National Institute of Mental Health recommend individualized treatment planning, fMRI-guided theta burst stimulation, and ongoing monitoring of cognitive side effects to maintain a safe profile.
Reflecting on TMS Therapy Safety
TMS therapy stands out as a safe, non-invasive option for mental health treatment, particularly for those struggling with treatment-resistant depression. Its minimal side effects and outpatient nature make it accessible and convenient. While risks exist, they are rare and manageable under expert care.
If you or a loved one wrestle with depression that hasn’t eased with medications or talk therapy, TMS could be a promising path worth exploring. You can learn more or schedule a thorough evaluation by visiting TMS of Tennessee. Taking that next step means informed choices and a potential new chapter in managing your mental health.
References
- https://www.cms.gov/medicare-coverage-database/view/lcd.aspx?lcdid=36469&ver=24