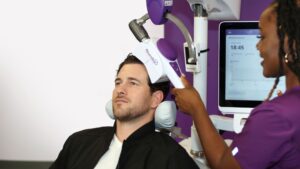
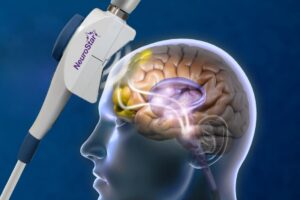
Transcranial Magnetic Stimulation (TMS) can lead to full remission of depression for a meaningful share of patients, especially those who have not responded well to medication.
Clinical trials and real-world data consistently show that TMS is a safe, evidence-based option with remission rates that are both measurable and medically significant.
While it does not work for everyone, many patients experience a return to a state where symptoms no longer interfere with daily life. Understanding how protocol, history of treatment, and diagnosis shape these outcomes can help you set realistic expectations, so keep reading to see how this may apply to you.
Key Takeaways
- Remission rates are strongly tied to depression severity and treatment resistance.
- Different TMS protocols, like theta burst stimulation, can influence outcomes.
- Real-world data confirms that remission is often a durable, lasting state.
What Does “Remission” Actually Mean in TMS?
In TMS treatment for major depressive disorder (MDD), remission has a very specific medical meaning. It is not just “feeling a little better” or having a few good days.
Clinically, remission means your symptoms have improved to the point that you no longer meet the criteria for major depression, based on structured assessment tools, not just impression or mood, a threshold reached by about 36% of patients in controlled rTMS trials compared with 8% receiving sham stimulation [1].
The most widely used tool is the Hamilton Depression Rating Scale (HDRS). On the 17‑item version, a score of 10 or below is commonly used to define remission.
Other validated scales, such as the Beck Depression Inventory (BDI), are used in a similar way. These instruments allow your clinician to track progress over time and to determine whether you have reached a true remission rather than a partial response.
From a patient perspective, remission usually feels like getting your life back. Energy, interest, and motivation begin to normalize. Daily tasks no longer feel overwhelming, and emotional stability improves in a sustained way, not just in brief windows.
Clinically, remission in TMS means:
- Standardized measurement
- HDRS ≤ 10 (17‑item scale) is a common remission cutoff.
- Tools like BDI support the same goal: goal tracking of symptoms.
- Functional recovery
- Return to work or school responsibilities.
- Re‑engagement with family, social life, and personal routines.
- Clear treatment endpoint
- Signals a successful TMS course.
- Guides decisions about maintenance strategies or follow‑up care.
The Clinical Factors That Shape Your Remission Odds

When we talk about remission with TMS, we’re really talking about how your specific clinical story shapes the numbers. TMS outcomes are not random; they follow patterns we see over and over again in the data.
Several key factors tend to influence your chances of remission:
- Severity of your current episode
- Patients with mild to moderate depression often have higher remission rates, in some studies reaching 50–60% or more.
- Those with severe or long-standing treatment‑resistant depression (TRD) usually see lower remission rates, more in the 19–30% range.
- This does not mean TMS is “not worth it” for severe cases, but it does help set honest expectations.
- Level of treatment resistance
- If you’ve tried two or more adequate antidepressant trials without enough benefit, you meet criteria for TRD.
- TMS is FDA‑cleared specifically for this group, but the more failed trials you’ve had, the harder remission tends to be to achieve.
- Comorbid psychiatric conditions
- Co‑occurring anxiety disorders, PTSD, or OCD can affect remission rates and may slow the response.
- That said, some patients see parallel improvement in both depression and anxiety symptoms with TMS.
- Early response to treatment
- A noticeable improvement by about the 10th session is a promising sign.
- Early responders are statistically more likely to reach full remission by the end of the course.
Taken together, these factors help your clinician estimate your remission odds and tailor a TMS protocol that fits your specific clinical profile, rather than relying on averages alone.
Protocol Variations and Their Impact
The way TMS is delivered has a direct impact on remission rates, and this comes down to both where and how the brain is stimulated.
“The most widely used approach is high-frequency repetitive TMS (rTMS) over the left dorsolateral prefrontal cortex (L-DLPFC). In clinical studies, this method generally shows response rates around 22–45% and remission rates around 16–22%, a pattern also reflected in clinical programs built around NeuroStar Advanced TMS Therapy.
Another established option is low‑frequency rTMS over the right DLPFC (R‑DLPFC), which appears to offer similar effectiveness, just with a different stimulation pattern and target side.
Newer protocols are designed to be more efficient while keeping outcomes comparable. Theta Burst Stimulation (TBS) delivers pulses in brief, patterned bursts that mimic natural brain rhythms.
It can be used as intermittent TBS (iTBS) or continuous TBS (cTBS). The main practical advantage is time: iTBS sessions usually last about three minutes, instead of the 20–40 minutes needed for a standard rTMS session, yet studies show similar response and remission rates to conventional protocols.
There is also growing interest in accelerated TMS (aTMS), where many sessions are given in a single day over a shorter course.
Early research on some TMS protocols has shown very high remission rates, in some small cohorts reported up to 90%, suggesting the possibility of faster and more robust improvement for selected patients, though this approach is still being actively studied and is not yet the standard everywhere.
- High-Frequency rTMS: The standard approach, with well-established remission data.
- Theta Burst Stimulation: A shorter-duration protocol with comparable efficacy.
- Accelerated TMS: An intensive protocol showing promise for higher remission rates.
Real-World Data Versus Controlled Trials

You get a very different view of treatment when you compare what happens in a tightly run study to what happens in a real clinic with real patients and real complications.
Clinical trials and everyday practice are both useful, but they answer different questions. One asks, “Can this work under ideal conditions?” The other asks, “Does this still work when life is messy?”
1. Evidence From Controlled Clinical Trials
Clinical trials are designed to test efficacy under controlled conditions. That means:
- Careful, standardized protocols
- Strict inclusion and exclusion criteria
- Close monitoring of side effects and adherence
In many of these trials, patients with complex medical or psychiatric comorbidities are excluded. For example:
- Significant medical illnesses
- Unstable psychiatric conditions
- Certain medications or treatment histories
So, the population is “cleaner” than what we see in normal practice. That’s useful for isolating the true effect of rTMS.
Findings from these controlled trials:
- Active rTMS reliably outperforms sham (placebo) stimulation.
- Meta-analyses show:
- Patients receiving active rTMS are about 2.8 times more likely to achieve remission compared with sham.
- Remission rates:
- About 36% with active rTMS
- About 8% with sham
This pattern tells us that rTMS has genuine antidepressant effects that go well beyond placebo in a controlled research setting.
2. Evidence From Real-World Clinical Practice
Real-world effectiveness is what we see in clinics such as TMS of Tennessee, where patients are not so carefully filtered.
Typical real-world patients often have:
- Multiple medical comorbidities
- Long histories of treatment-resistant depression
- Prior medication failures
- Social stressors and functional impairment
- Mixed psychiatric profiles
This is much closer to what you and I see in day-to-day practice.
Despite this higher level of complexity, real-world data has been encouraging:
- Outcomes in naturalistic studies are broadly in line with clinical trials.
- One naturalistic study reported that:
- 58% of patients who achieved remission with TMS maintained remission three months after finishing their treatment course, similar to results seen in structured treatment pathways such as TMS accelerated.
That kind of durability matters. Depression is not just an acute episode for many patients; it’s often a chronic, relapsing condition. Seeing remission maintained over several months suggests that TMS can provide more than a brief lift.
3. What This Means Clinically
From a medical perspective, we are aiming for more than short-term symptom relief. The goals are:
- Achieving remission
- Maintaining wellness
- Reducing relapse risk
- Improving daily functioning and quality of life
Putting the data together:
- Controlled trials show that rTMS has clear antidepressant efficacy under ideal, highly selected conditions.
- Real-world studies show that, even in more complex and less predictable patient populations:
- Response and remission rates remain clinically meaningful.
- A significant part of patients can maintain remission for months after treatment.
For depression treatment, that combination,strong evidence in trials and solid performance in everyday practice, supports TMS as a serious, durable option for patients who have not responded adequately to medication alone.
A Realistic Look at the Numbers

So, what is the remission rate for TMS? A blanket number is misleading, but looking at the range is informative.
For patients with treatment-resistant depression, remission rates typically fall between 30% and 60%, depending on the factors discussed, with some real-world inpatient comparisons reporting 44.9% remission using twice-daily rTMS and 45.4% using once-daily protocols [2].
The NeuroStar Advanced TMS system, which we use, cites a 62% remission rate based on its large clinical dataset, aligning with outcomes frequently observed in clinics that integrate comprehensive programs like TMS therapy for depression.
It’s also helpful to consider response rates, which are higher. A “response” is typically defined as a 50% or greater reduction in depression scale scores. Many patients who respond but do not fully remit still experience a life-changing improvement in their symptoms.
The effect size of TMS, a statistical measure of its power, is often reported as a Hedges’ g of around 0.55 to 0.70. This places it in the medium-to-large range for therapeutic interventions, confirming its significant impact on depressive symptoms.
FAQ
What affects the remission rate for people using repetitive transcranial magnetic stimulation?
Many people want to know what shapes their chances of getting better with repetitive transcranial magnetic stimulation.
Doctors often look at things like early response predictor signs, depression severity TMS patterns, and how major depressive disorder TMS treatment fits the person’s needs. Real world TMS efficacy also helps explain why some patients improve faster than others.
How do rTMS depression remission numbers differ for treatment resistant depression TMS patients?
People with treatment resistant depression TMS often ask if their remission chances differ from others.
rTMS depression remission numbers depend on factors like TMS response rates, HDRS remission criteria, and how well patients handle daily TMS sessions. Many also track BDI score reduction or Hamilton depression rating scale changes to see if symptoms move in the right direction.
What do researchers study in TMS clinical trials meta-analysis to understand remission patterns?
Researchers often check TMS clinical trials meta-analysis papers to understand how patients respond over time. They compare things like dorsolateral prefrontal cortex stimulation approaches, high frequency rTMS versus low frequency rTMS, and theta burst stimulation methods.
Some studies also include TMS sham comparison results to see how much improvement comes from true antidepressant effects TMS provides.
Can major depressive disorder TMS treatments use personalized TMS targeting to improve outcomes?
Many patients ask if personalized TMS targeting can raise their chances of getting better. Some clinics study brain network TMS features, fMRI guided TMS, and L-DLPFC stimulation or R-DLPFC stimulation to find better spots for treatment.
These methods may help people with major depressive disorder TMS by supporting stronger response likelihood TMS patterns in everyday care.
How long do TMS durability remission results last for people who respond well to treatment?
People who feel better after TMS often wonder how long results last. TMS durability remission depends on factors like 3 month remission maintenance, sustained TMS effects, and how TMS follow up remitters manage daily life.
Mild depression remission may last longer, while severe depression TMS patients might need extra support or adjunctive TMS medication to keep symptoms down.
Your Path to Remission
The data on TMS remission rates is not just a collection of statistics. It is a map of realistic outcomes for individuals seeking a way out of treatment-resistant depression.
Remission is an achievable goal, shaped by your specific clinical profile and by the advanced technology behind modern TMS protocols. The evidence supports that this non-drug, non-invasive therapy offers a substantial opportunity for a lasting return to wellness.
If you see yourself in the description of someone who has not found relief through traditional antidepressants, TMS represents a validated next step. The process usually begins with a careful clinical consultation to determine whether you are an appropriate candidate. From there, a personalized treatment plan is developed around your history, your symptoms, and your goals.
The potential for remission is real, supported by more than a decade of clinical use and ongoing research.
If you’d like to see how these general principles might apply to your own situation, the next step is a professional evaluation with a TMS provider.
You can schedule a free consultation with TMS of the Carolinas to discuss NeuroStar Advanced TMS Therapy and whether it may be right for you by visiting TMS of Tennessee.